The Hidden Cycle Behind Chronic Sinusitis
Many people think of sinus infections as isolated events: a bad cold, a round of antibiotics, then life moves on.
But for some patients, recurrent sinus infections slowly evolve into something much more complex. What begins as episodic can gradually change the biology of the nasal lining itself, leading to chronic sinusitis - a condition driven not just by infection, but by immune system dysfunction and persistent inflammation.
Acute sinusitis is usually triggered by a viral upper respiratory infection. The lining of the nose and sinuses swells, mucus flow thickens and slows down, and bacteria may overgrow secondarily. Most people recover. But when these episodes happen repeatedly, the immune system can become stuck in a prolonged state of activation.
Over time, the immune response begins to shift. Instead of simply reacting to an infection and then calming down, inflammatory signals continue circulating in the nasal tissue. Cells within the immune system release chemical messengers that recruit more inflammatory cells, increase mucus glands, and weaken the integrity of the sinus lining. In some patients, this can eventually lead to mucosal remodeling - a process where the tissue itself changes structure.
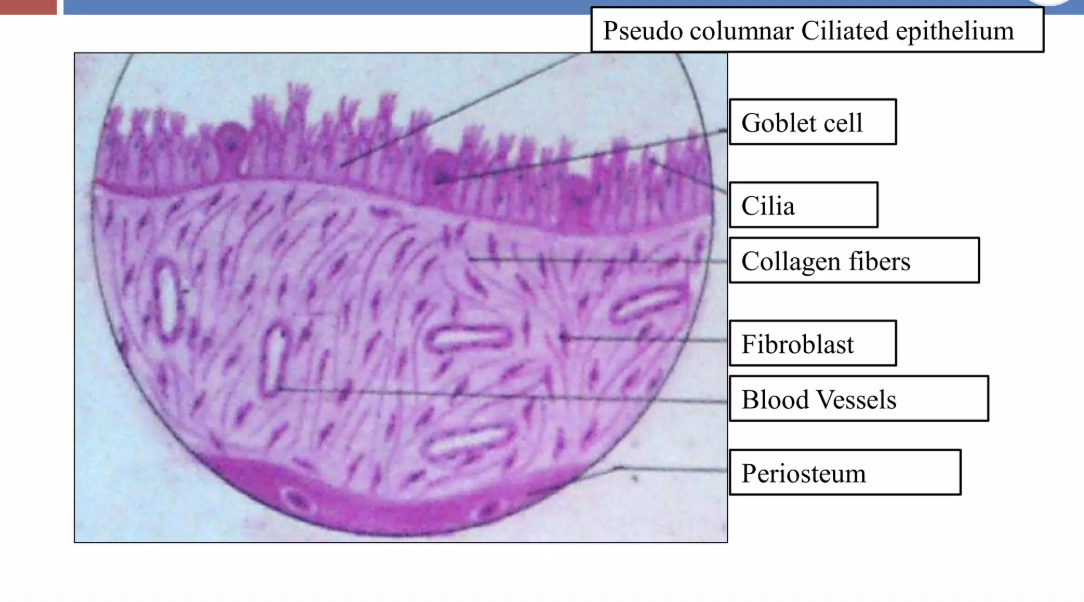
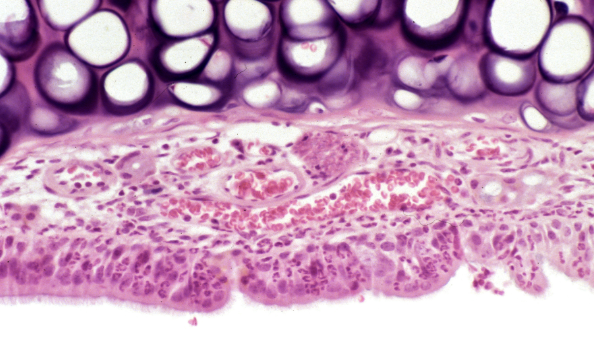
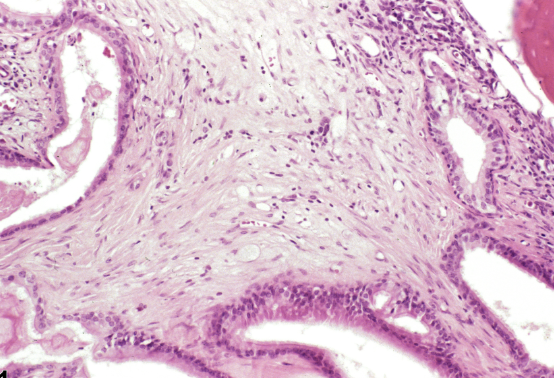
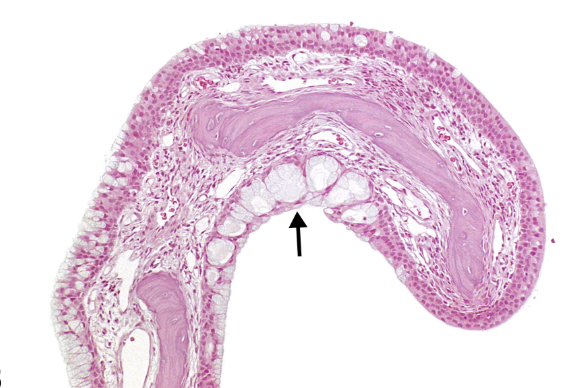
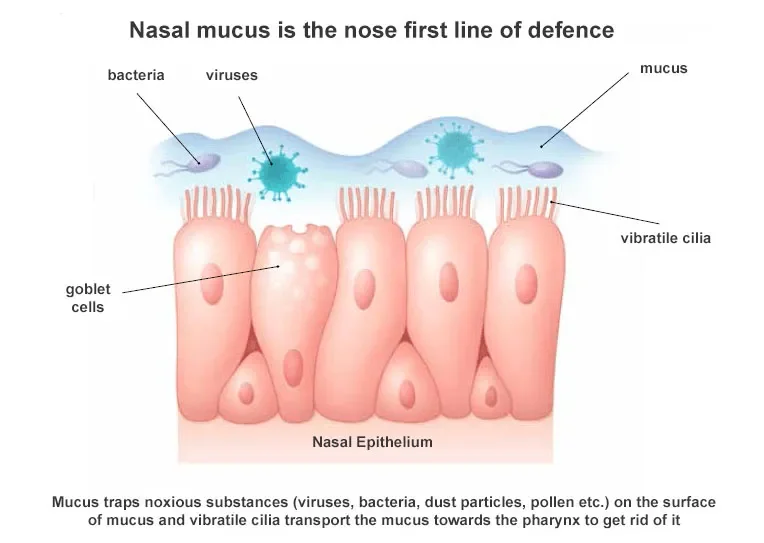
This remodeling may include thickened sinus lining, impaired ciliary function (the tiny “sweepers” that move mucus), polyp formation, increased mucus gland density, and altered microbial balance within the nose and sinuses. At this stage, chronic sinusitis is no longer simply “recurrent infections.”
The environment inside the sinuses has fundamentally changed.
And recurrent viruses are not the only thing that can drive these chronic inflammatory changes. Environmental allergies, poor air quality, smoke exposure, mold, occupational irritants, and even chronic exposure to chemical fragrances or cleaning products can repeatedly stimulate and injure the nasal lining.
Think of your nasal and sinus mucosa as a protective barrier. Its job is to filter particles, regulate moisture, trap pathogens, and coordinate immune defense. But the more this barrier becomes inflamed or damaged, the more vulnerable it becomes. Over time, even a relatively routine cold virus may be more likely to trigger severe swelling, mucus stagnation, and a prolonged sinus infection.
Importantly, the immune system does not operate in isolation. The body’s inflammatory burden is influenced by sleep quality, stress physiology, metabolic health, environmental exposures, physical activity, and even breathing patterns. That is why an integrative approach to chronic sinusitis looks beyond the sinuses alone.
Sleep plays a major role in immune regulation and tissue recovery. Poor sleep is associated with increased inflammatory signaling and impaired immune resilience. Nutrition matters because the foods we eat influence oxidative stress, gut microbiome diversity, and systemic inflammation. Physical activity supports circulation, immune surveillance, stress regulation, and nitric oxide production.
Nasal breathing itself is also important. The nose is not just a passive airway - it warms, humidifies, filters air, and produces nitric oxide, a molecule involved in vascular and immune function. Chronic mouth breathing can worsen dryness, inflammation, and poor breathing mechanics.
And for some patients, targeted supplements or herbals may provide additional support. Depending on the individual, this may include therapies aimed at improving mucosal health, supporting immune balance, reducing oxidative stress, or promoting healthier inflammatory signaling.
Chronic sinusitis is rarely caused by one thing alone - which is why lasting improvement often requires an integrative approach.
If you want to learn the top overlooked drivers that keep people stuck in recurrent sinus infections and chronic sinus inflammation, check out my free guide here.